Approach to fluid electrolyte disorders in the Emergency Department
Cellular cation K: 150, Mg: 40 mEq/L; Cellular anion P: 120 mEq/L
Extracellular cation Na: 142, Cl: 104 mEq/L; Extracellular anion HCO3: 30 mEq/L
SERUM OSMOLALITY: (2 x Na) + (glucose/18) + (BUN/2.8)
The reason for multiplying Na by two is that the total of Cl and HCO3 is approximately equal to Na.
Normal serum osmolality is between 275-295.
Volume loss triggers two mechanisms:
- Activation of the pituitary region; ADH increases, and renal water retention increases.
- Increased renal renin secretion, increased aldosterone secretion from the adrenal gland, and increased renal Na retention.
POTASSIUM
When serum pH decreases, serum K increases because K shifts from the cellular to the vascular space. A 0.1 decrease in pH increases K by 0.5. Similarly, a 0.1 increase in pH decreases serum K by 0.5.
HYPERKALEMIA
Hyperkalemia is most commonly encountered in end-stage kidney disease patients.
SYMPTOMS: Weakness, ascending paralysis, respiratory failure.
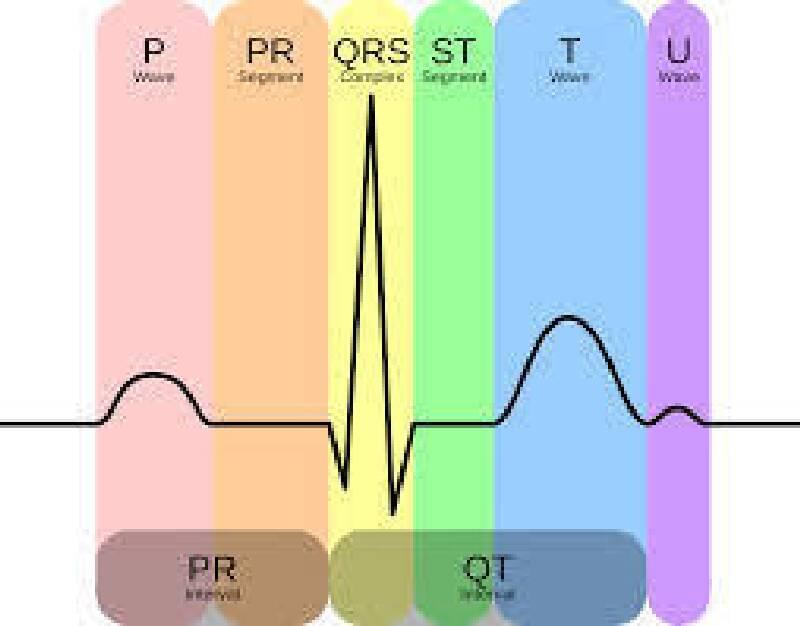
EKG FINDINGS:
T wave peaking Prolonged PR interval (1st-degree heart block) Widening of QRS complex Flattening of P wave Deepening of S wave Merge of S and T waves (short QT) Idioventricular rhythm Asystole
Note: In a normal EKG record, the speed is 25 mm/s, and 1 small square (1 millimeter) corresponds to 0.04 seconds;
- P wave should be < 0.10 s or < 2.5 mm
- PR interval should be between 0.12 s and 0.20 s or 3-5 mm (3-5 small squares)
- QRS complex should be between 0.06 s and 0.10 s or 1.5-2.5 mm
- QT interval should be between 0.33 s and 0.42 s or 8-10.5 mm
(Hyperkalemic Periodic Paralysis) Not: CONDITIONS LEADING TO K SHIFT FROM INTRA- TO EXTRACELLULAR SPACE:
- Insulin deficiency
- Acidosis
- Beta-blockade
- Digitalis toxicity
- Hyperkalemic periodic paralysis
- Intense exercise
TREATMENT:
Mild Elevation (5-6 mEq/L) Removing potassium from the body is sufficient;
- Diuretics: Furosemide 40-80mg iv
- Resins: Kayexalate (cation exchange resins), 15-30 gr PO and rectal (with sorbitol)
Moderate Elevation (6-7 mEq/L)
- Glucose – Insulin therapy
- Sodium Bicarbonate; 50 mEq iv over 5 minutes (especially in patients with renal insufficiency, less effective than other treatment methods)
- Nebulized Albuterol (Salbutamol); 10-20 mg nebulized Ventolin over 15 minutes.
Severe Elevation (> 7 mEq/L and association with toxic EKG changes) In severe elevation situations, both pushing K into cells and increasing K excretion are required. Shifting K into cells is a fast and effective treatment but is temporary. Treatment should be repeated in cases of rebound K elevation.
K Intracellular Shift:
- %10 Calcium Gluconate; 10-20ml iv over 2-5 minutes (onset 1-3 minutes, duration 30-50 minutes) or %10 Calcium Chloride; 5-10ml iv over 2-5 minutes
Note: 10ml % 10 Ca Gluconate contains 93 mg Elemental Ca 10ml % 10 Ca Chloride contains 273 mg Elemental Ca
- Sodium Bicarbonate; 50 mEq over 5 minutes
- Glucose + Insulin
- Nebulized Albuterol
B. Excretion of K from the Body
- Diuresis
- Kayexalate enema 15-50gr + Sorbitol, oral or rectal
- Dialysis
HYPOKALEMIA
It refers to a serum K level < 3.5 mEq/L.
ETIOLOGY:
Gastrointestinal losses; Diarrhea Renal losses: Hyperaldosteronism, severe hyperglycemia, diuretics that cause K excretion, certain penicillin antibiotics Intracellular shift; Alkalosis Malnutrition
NOTE: The main cause of hypocalcemia accompanying vomiting is metabolic alkalosis. The effect of active K loss is low. Additionally, volume loss increases aldosterone secretion, leading to Na and HCO3 retention and K excretion.
SYMPTOMS: Flaccid paralysis, hypoventilation, paralysis of the ileus
EKG FINDINGS:
- U wave
- Flattening of the T wave
- Prolongation of the PR interval
- Widening of the QRS complex
TREATMENT:
Severe Elevation (> 7 mEq/L and association with toxic EKG changes) The preferred K-lowering agent is loop diuretics. If the glomerular filtration rate is impaired, a thiazide-type diuretic may be added.
- Loop Diuretics (Furosemide 40-80 mg iv)
- Thiazide Diuretics (Chlorthalidone 15-50 mg PO)
- Diuretic administration is started with the slow iv route and a low dose in patients using ACE inhibitors, ARBs, and NSAIDs, especially in those with renal insufficiency.
Caution: Diuretics cause K loss by increasing its urinary excretion. Therefore, they should not be used in hypokalemia cases due to mineralocorticoid excess. Otherwise, further deterioration of hypokalemia may occur.
HYPERCALCEMIA
It refers to a serum Ca level > 10.5 mg/dl.
ETIOLOGY:
Primary hyperparathyroidism Malignancy Granulomatous diseases (sarcoidosis, TB) Familial hypocalciuric hypercalcemia (FHH) Medications (thiazide diuretics, lithium) Vitamin D intoxication Thyrotoxicosis
SYMPTOMS: Polyuria, Polydipsia, Dehydration, Constipation, Nausea/Vomiting, Abdominal Pain, Decreased Appetite, Weakness, Fatigue, Confusion
EKG FINDINGS:
Shortened QT interval (Ca increases the speed of depolarization of pacemaker cells)
TREATMENT:
It is not required in asymptomatic patients.
Treatment is indicated in the following situations:
Symptomatic cases Severe hypercalcemia (Ca > 14 mg/dl) Hypercalcemia associated with kidney disease Cases with a high risk of progression
Hydration: Intravenous saline infusion 200-300 mL/h. (Isotonic solution) Furosemide: Diuresis induced by saline can result in calcium loss. For this reason, furosemide 20-40 mg iv can be used.
Intravenous Bisphosphonates: Zoledronic acid 4 mg iv over 15 minutes.
- Pamidronate
- Alendronate
Calcitonin: It is not used alone due to its short duration of action.
Dialysis: Especially in cases of volume overload, uremia, refractory to other treatments, and hypercalcemia-associated kidney disease.
HYPOCALCEMIA
It refers to a serum Ca level < 8.5 mg/dl.
ETIOLOGY:
Hypoparathyroidism Vitamin D deficiency Malabsorption Renal failure Acute pancreatitis Alkalosis Pseudohypoparathyroidism Magnesium deficiency
SYMPTOMS: Increased neuromuscular excitability, muscle cramps, laryngospasm, carpopedal spasm, Chvostek’s sign (facial muscle spasm upon tapping the facial nerve), Trousseau’s sign (carpal spasm when the blood pressure cuff is inflated above systolic pressure).
EKG FINDINGS:
Prolonged QT interval T-wave abnormalities ST-segment depression
TREATMENT:
- Intravenous Ca gluconate is preferred in severe symptomatic hypocalcemia.
- Oral Ca and Vitamin D supplementation for chronic management.
- Correcting magnesium deficiency if present.
- Treatment of the underlying cause.
Note: The initial amount of Ca gluconate is calculated as follows: 0.1 x weight (kg) x (8.8 – serum Ca). The calculated amount is diluted in 100 ml of 5% dextrose solution and administered over 10-20 minutes. If there is no improvement, it can be repeated every 1-2 hours. Long-term management includes oral calcium and vitamin D supplementation.
I hope this information is helpful. If you have any more questions or need further clarification, feel free to ask.

